Blog
The Importance of Stretching and Mobility Exercises for Injury Prevention
Think stretching is just for athletes or warming up before a workout? Think again. Stretching and mobility exercises are key tools we use to help patients in Clarke, Oconee and Watkinsville, Madison, and Morgan counties stay injury-free, move better, and stay active...
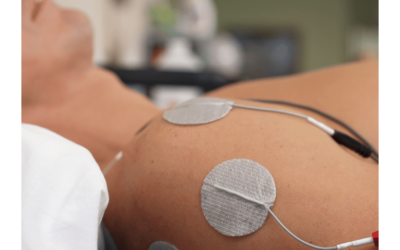
Neubie Therapy: A Game-Changer for Speeding Up Recovery
What if your recovery could happen faster, with less discomfort and more control over your results? That’s exactly what Neubie therapy brings to the table. This advanced electrical stimulation technology is changing the way we help patients in Clarke, Oconee, Madison,...
How Physical Therapy Supports Recovery from Rotator Cuff Injuries
Shoulder pain from a rotator cuff injury can make simple tasks like lifting a cup or reaching for a seatbelt feel impossible. We help patients recover from rotator cuff injuries with targeted treatment plans that improve mobility, reduce pain, and restore upper body...
Rehabilitation Strategies for Total Joint Replacement Patients
Recovering from total joint replacement doesn’t just happen—it takes a strategic, individualized approach tailored to your body and your goals. Our therapists specialize in helping patients recover mobility, reduce pain, and return to the life they love after hip,...
The Impact of Posture on Spine Health and How PT Can Help
We don’t always think about how we sit, stand, or move throughout the day — until pain starts to creep in. Poor posture is one of the most common contributors to neck, back, and shoulder pain. The good news? Physical therapy offers effective solutions to correct...
Preparing High School Athletes for the Season with Neubie
Every athlete wants to step into the season stronger, faster, and ready to compete. But preparing the body for peak performance takes more than just practice on the field. It takes smart, science-backed training designed to build resilience and prevent...
Neck and Shoulder Pain Treatment That Restores Comfort and Mobility
Neck and shoulder pain can turn everyday tasks into painful challenges — from looking over your shoulder while driving to simply reaching for a coffee cup. When discomfort lingers or worsens, physical therapy offers real solutions that target the root of the...
Managing Chronic Back Pain: Effective Physical Therapy Approaches
Chronic back pain can feel like it controls your life. From getting out of bed in the morning to working, driving, or exercising, back pain impacts everything. But physical therapy offers hope. With evidence-based care and advanced techniques, we help our...
Neuromuscular Dysfunction: Common Causes and PT Solutions
Neuromuscular dysfunction can significantly impact mobility, strength, and overall quality of life. Whether caused by injury, disease, or aging, these conditions affect the way muscles and nerves communicate, leading to weakness, pain, and movement...
How to Improve Balance and Prevent Falls for Older Adults
Falls are one of the leading causes of injury and loss of independence among older adults. As we age, changes in muscle strength, coordination, and reflexes can increase the risk of falls. However, with the right interventions, balance can be improved, and falls...